Management of persistent hyperglycemia in type 2 diabetes mellitus. Literature review current through. Jun 2. 01. 7. Monotherapy with metformin is indicated for most patients, and insulin may be indicated for initial treatment for some . Although several studies have noted remissions of type 2 diabetes mellitus that may last several years, most patients require continuous treatment in order to maintain normal or near- normal glycemia.
- Inflammation (from Latin inflammatio) is part of the complex biological response of body tissues to harmful stimuli, such as pathogens, damaged cells, or irritants.
- Maria Fernandez has received nearly a half million dollars from the egg industry and writes papers like “Rethinking dietary cholesterol.” She admits that eggs can.
- Live your happiest and healthiest life ever, compliments of these M.D.
- This topic contains 278 study abstracts on Clogged Arteries indicating that the following substances may be helpful: Arginine, Omega-3 Fatty Acids, and Garlic.
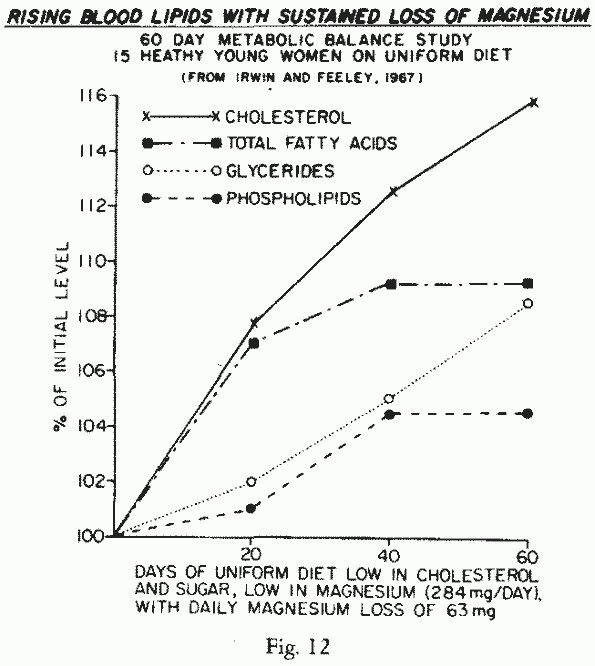
- Green vegetables such as spinach are good sources of magnesium, which is contained in the chlorophyll molecule. Some legumes (beans and peas), nuts.
- Free ebook: Machiavelli's Laboratory "Ethics taught by an unethical scientist" 12,000 BIOMEDICAL ABBREVIATIONS This page is provided "as is", without warranty of any.
- Below is an approximation of this video’s audio content. To see any graphs, charts, graphics, images, and quotes to which Dr. Greger may be referring, watch the.
Bariatric surgical procedures in obese patients that result in major weight loss have been shown to lead to remission in a substantial fraction of patients. Regardless of the initial response to therapy, the natural history of most patients with type 2 diabetes is for blood glucose concentrations to rise gradually with time. Treatment for hyperglycemia that fails to respond to initial monotherapy and long- term pharmacologic therapy in type 2 diabetes is reviewed here. Options for initial therapy and other therapeutic issues in diabetes management, such as the frequency of monitoring and evaluation for microvascular and macrovascular complications, are discussed separately. We are aware that this A1. C goal is not appropriate for all patients, especially older adults and those with comorbid conditions or limited life expectancy.
Target A1. C goals in patients with type 2 diabetes should be tailored to the individual, balancing the improvement in microvascular complications with the risk of hypoglycemia. Glycemic targets are generally set somewhat higher for older patients and those with comorbidities or a limited life expectancy and little likelihood of benefit from intensive therapy. Glycemic targets are reviewed in more detail separately. An analysis from the United Kingdom Prospective Diabetes Study (UKPDS) found that 5. A1. C value . Whether patients with truly new- onset diabetes, identified through screening, behave similarly is unknown.
Among the factors that can contribute to worsening glycemic control are. The latter factor (ingestion of certain drugs) is particularly important in older patients who are taking multiple drugs. A population- based study of over 7. A1. C levels higher than ideal for years because changes in therapy to improve glycemic control were not made or were only made slowly . Adherence to algorithms that dictate changes in treatment at designated intervals and computerized decision aids may improve A1. C more efficiently than standard care . We favor basal insulin or sulfonylurea as the second step, and insulin is preferred for patients whose A1.

C is further from target (> 8. This algorithm, modified from the algorithm endorsed by the American Diabetes Association (ADA) in 2.
A1. C against adverse effects, side effects, and costs . Subsequent ADA recommendations have been less prescriptive and not provided guidance regarding the hierarchy of medications (figure 2) . In a meta- analysis of 1. A1. C, body weight, lipid profiles), combination therapy decreased A1. C levels more than monotherapy by approximately 1 percentage point . Most combinations similarly reduce A1.
C . In one meta- analysis, there was moderate evidence favoring metformin plus a glucagon- like peptide- 1 (GLP- 1) agonist over metformin plus a dipeptidyl peptidase- 4 (DPP- 4) inhibitor for reducing A1. C levels . The glycemic efficacy of some of the combinations is reviewed below.
Initial treatment of patients with type 2 diabetes mellitus includes education, with emphasis on lifestyle changes including diet, exercise, and weight reduction when. What to Expect From Weight Loss Surgery; Health Risks of Obesity; Prescription Weight Loss Drugs; Is Weight Loss Surgery Right for You? What Is Gastric.
We favor insulin or sulfonylureas as the preferred second- line agents because of efficacy, side- effect profile, long- term safety, and relative cost (algorithm 1). Repaglinide is principally metabolized by the liver, with less than 1. Thus, it can be used safely in patients with chronic kidney disease.
A prior history of myocardial infarction or stroke might also favor choosing liraglutide as the second drug to be added to metformin, based on the results of the liraglutide and cardiovascular outcomes study. Although both liraglutide and empagliflozin appear to decrease cardiovascular morbidity and mortality in patients with type 2 diabetes and established CVD, the balance between benefits and risks have not been examined in the long term.
In addition, there are few data on benefits and risks in patients who have not had a major CVD event. However, the modest glucose- lowering effectiveness, expense, and limited long- term clinical experience may temper enthusiasm for these drugs. However, in certain clinical settings, such as especially high risk for hypoglycemia or intolerance of or contraindications to sulfonylureas, a thiazolidinedione may be added. As an example, in a patient who would be at particularly high risk if hypoglycemia occurred (eg, a construction worker) and who has inadequate glycemic control on metformin (A1. C > 7 but < 8. The use of rosiglitazone is not recommended, because of the greater concern about its atherogenic lipid profiles and a potential increased risk for cardiovascular events . In 2. 01. 0, the European Medicines Agency suspended sales of rosiglitazone, owing to concern regarding cardiovascular safety and the availability of alternative therapies, including pioglitazone, that do not have the same concerns.
In 2. 01. 0, the US Food and Drug Administration (FDA) imposed marked restrictions on the prescribing of rosiglitazone because of concerns about increased risk of acute myocardial infarction and cardiovascular deaths. These restrictions were largely removed by the FDA in 2. In 2. 01. 1, the French and German Medicines Agencies suspended the use of pioglitazone because of the potential increased risk of bladder cancer and the concern that the overall risks of pioglitazone exceed its benefits.

The European Medicines Agency, the FDA, and Japanese regulators withheld action on pioglitazone pending results of ongoing review of the data. For patients who are doing well on these particular doses, the combination tablets offer the convenience of taking fewer pills. However, if the patient needs the dose of either drug to be changed independent of the other drug, then a fixed combination is unhelpful. In addition, the cost of the brand name combinations is substantially greater than taking the generic components individually.

Sulfonylurea monotherapy failure — In individuals with contraindications to metformin, sulfonylureas are often first- line therapy. Shorter- acting sulfonylureas, such as glipizide, are less likely to cause hypoglycemia than the older, long- acting sulfonylureas and therefore are the preferred sulfonylureas, especially in older patients. In patients who are intolerant or cannot take metformin for any reason and who have an A1. C that is < 8.
The choice of therapy should be individualized based upon patient characteristics, preferences, and costs. Options include thiazolidinediones, DPP- 4 inhibitors, GLP- 1 agonists, sodium- glucose co- transporter 2 (SGLT2) inhibitors, alpha- glucosidase inhibitors, and insulin.
All of these medications have advantages and disadvantages (table 2), and all of the newer medicines that are not available in generic form are relatively expensive. Hypoglycemia remains a risk when any of these medications are used in combination with a sulfonylurea.
In general, sulfonylureas are tapered and stopped if insulin is added and especially if the insulin regimen includes preprandial rapid- acting insulin. GLP- 1 receptor agonists may be appropriate to use in combination with sulfonylureas in certain clinical settings, eg, when weight loss is a primary consideration and the A1. C level is close to target. A prior history of myocardial infarction or stroke might also favor choosing liraglutide as the second drug, based on the results of the liraglutide and cardiovascular outcomes study. Empagliflozin may also be considered in patients with established CVD.
DPP- 4 inhibitors or SGLT2 inhibitors can be considered as add- on drug therapy to sulfonylureas in patients who have contraindications to metformin and pioglitazone. However, the modest glucose- lowering effectiveness, expense, and limited long- term clinical experience with these drugs temper our enthusiasm. In patients on sulfonylureas and metformin who are starting insulin therapy, sulfonylureas are generally tapered and discontinued, while metformin is continued. Part of the rationale for combination metformin and insulin therapy is that by suppressing hepatic glucose production, the patient can retain the convenience of oral agents while minimizing total insulin requirements and therefore the degree of hyperinsulinemia . It is reasonable to try a GLP- 1 agonist before starting insulin in patients who are close to glycemic goals, who prefer not to start insulin, and in whom weight loss or avoidance of hypoglycemia is a primary consideration. In randomized trials comparing GLP- 1 agonists with insulin in patients with type 2 diabetes inadequately controlled with metformin and sulfonylurea, there were similar reductions in A1.
C in the two groups. However, in some of the trials, the insulin was often not adjusted as aggressively as it could or should have been based on labeling and usual clinical practice.
These trials are reviewed separately. This was illustrated in a study of 2. At study end (2. 4 weeks), improvements in A1. C (approximately 1.
However, insulin glargine was superior in reducing A1. C values when baseline A1. C values were > 9.
Although insulin glargine was associated with more hypoglycemic events, there were fewer overall adverse events, significant improvements in the serum lipid profile, and it was less expensive. Subjects treated with insulin glargine also reported greater improvements in several health- related, quality- of- life measurements . These findings, combined with the greater concern about adverse cardiovascular events with thiazolidinediones, particularly rosiglitazone, favor the addition of insulin glargine over rosiglitazone. This was demonstrated in a study of 1.
 RSS Feed
RSS Feed
